Innovation Roundup
A newsletter about innovation, technology, health economics, regulation and empathy in medicine (1/3/24)
Hi,
Some exciting news! Please join us for our inaugural innovation webinar series sponsored by the Frankel Cardiovascular Center on Friday January 5 at 9 AM EST.
This issue at a glance:
Barriers and facilitators to utilizing digital health technologies by healthcare professionals.
A method for LLMs to "deliberate" on responses to correct mistakes.
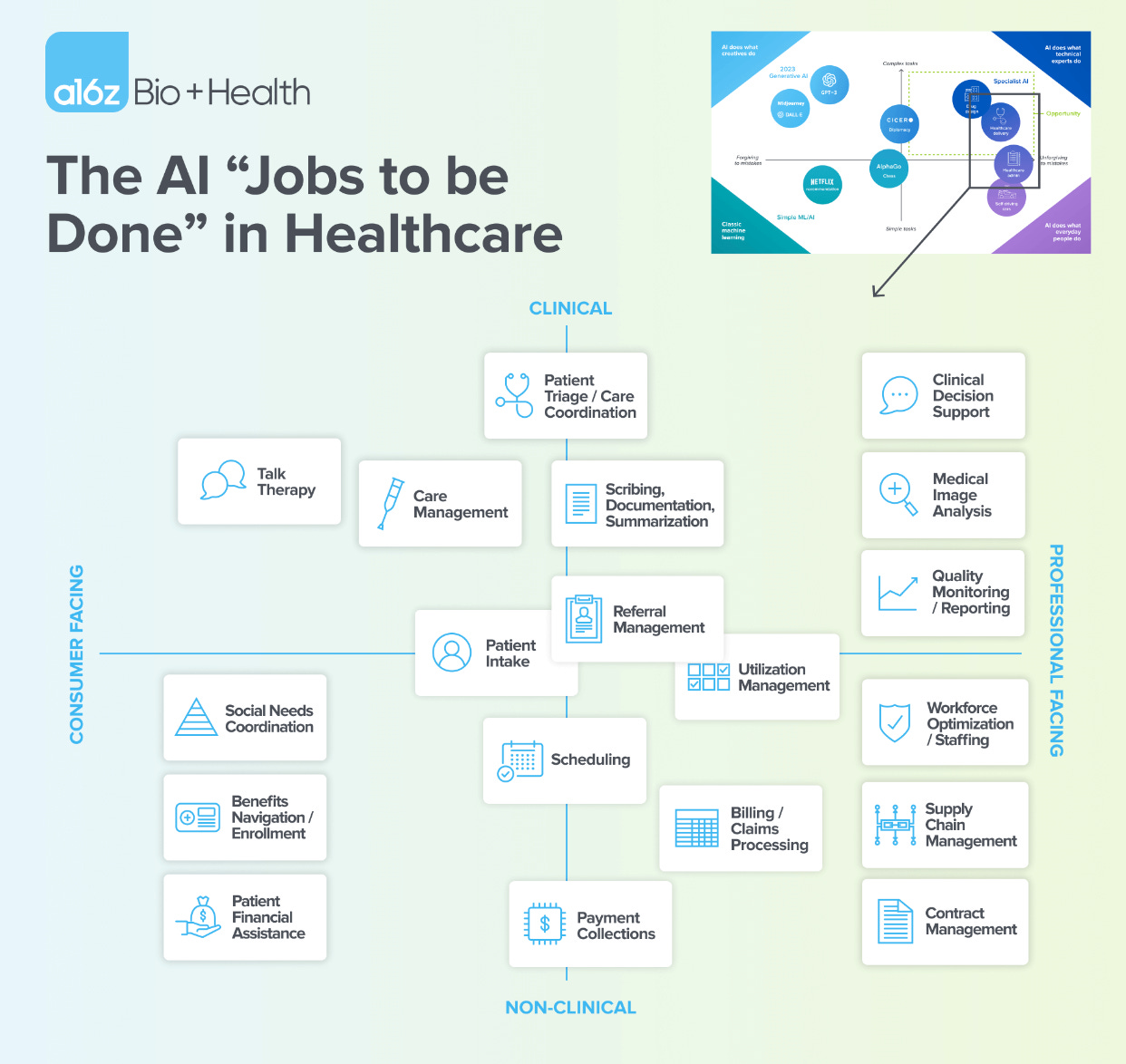
How to use Clay Christensen’s Jobs to be Done lens, along with an assessment of viable product wedges and business models, to see the most promising applications of AI in enterprise healthcare.
UnitedHealth faces class action lawsuit over algorithmic care denials in Medicare Advantage plans
Using eSTAR through the CDRH Portal to enhancing the quality of the premarket submissions and efficiency of premarket review
Enjoy,
Hamid
Science Roundup
Barriers and facilitators to utilizing digital health technologies by healthcare professionals
As we roll out our digital health clinic, one of the main areas of focus has been to make sure we identify the causes of lack of adoption and enrollment in our program and design specific ways to try to address them. We have observed that almost everybody wants to enroll in our program only about 60% actually end up enrolling. One thing that I have learned so far is that proper implementation and a systematic management approach, including strategic planning, resource allocation, and control and evaluation processes, is key for developing any successful program.
In this review, infrastructure and technical issues were the most frequently described barriers. This was related to limited or insufficient networks, lack of existing technologies, lack of devices, compatibility with daily workflow, connectivity speed, healthcare capacity of technology integration, interconnectedness, absence of standardized/harmonized systems at different facilities, limited access to electricity, and requirement of a functional database system. Not surprisingly technical issues seem to be the worst in rural and countryside regions. Counteracting connectivity-related barriers involves ensuring availability (especially in rural areas) and affordability, guaranteeing high-speed fiber connectivity, and increasing the number of reliable local networks.
Personal and psychological barriers included the healthcare professionals’ resistance to change, difficulty understanding the technology, perception of less human interaction, technophobia, ages, education levels, professional experience, low literacy, poor writing skills, linguistic features, adherence behavior, and fear of using particular health technology. Moreover, unwillingness, low expectations, skepticism from healthcare providers, and low motivation for compliance were also associated with personal barriers.
For counterbalancing these barriers, healthcare professionals’ perception of usefulness and willingness was a highly cited facilitator, characterized by the degree to which the employees believe that using specific digital health technologies would enhance their performance and the proportion of participants intending to utilize that technology. Furthermore, personal and psychological barriers could be addressed by using and adopting training programs and educational activities appropriately tailored to healthcare professionals’ needs and coverage of deficient abilities. Evidence shows that user-friendly design, intuitive system navigation, and easy-to-use interfaces are critical to improving overall product performance and facilitating data collection and input, data processing, and further analysis.
An important limiting factor for the broad use of digital health technologies is associated with healthcare workers’ concerns about increased workload and altered workflow, which could hinder the sustainability of the digital health technologies. Additionally, these newly implemented technologies would require additional purchase time and increased set-up, implementation, training, access, adaptation, and establishment stages. In addition, healthcare professionals commonly stressed that digital health technologies would impact the quality of delivered care, as recently trained professionals would need a longer time to convert acquired data into the implemented system. However, although time might be required to acquire the right skills and operating competencies, with adequate training, continuous technical support, and peer-to-peer collaboration, threats associated with increased time to complete a specific task are significantly reduced. Useful written guidelines, instructions, and handouts appear to be important facilitators that could be easily implemented. Likewise, incentives from government agencies and multi-sector organizations were shown to significantly improve digital health technologies’ effectiveness and chances of success in large-scale healthcare systems.
Legal- and ethical-related barriers were shown to be a relevant factor for healthcare providers, as privacy and security concerns, national legislation, jurisdiction, and the existence of unclear legal liability regarding response protocols would directly affect healthcare professionals. Possible interventions for these barriers are associated with the development of safer data storage systems, the establishment of requirements on safety and security in cooperation with healthcare professionals and patients, or the creation of an international legal framework and legislative norm, which would clarify security regulation policies that could help ensure patients’ privacy and confidentiality, as well as define healthcare professionals’ liabilities.
Chain-of-Verification Reduces Hallucination in Large Language Models
This paper suggest a method for LLMs to "deliberate" on responses to correct mistakes. Here is how
1) draft initial response
2) plan verification questions to fact-check the draft
3) answer questions independently to avoid bias from other responses
4) generate a final verified response
It turns out that by being more explicit about verifying questions, you can decrease hallucinations.
Industry Roundup
a16z AI jobs to be done in healthcare
Healthcare Economics and Policy Roundup
UnitedHealth faces class action lawsuit over algorithmic care denials in Medicare Advantage plans
The class action suit, filed on behalf of deceased patients who had a UnitedHealthcare Medicare Advantage plan and their families by the California-based Clarkson Law Firm, follows the publication of a STAT investigation Tuesday. The investigation, cited by the lawsuit, found UnitedHealth pressured medical employees to follow an algorithm, which predicts a patient’s length of stay, to issue payment denials to people with Medicare Advantage plans. Internal documents revealed that managers within the company set a goal for clinical employees to keep patients rehab stays within 1% of the days projected by the algorithm.
A brief history of Medicare advantage plan can be found here:
The federal government pays private insurance companies a capitated amount per enrollee, with the idea that the private market would be more cost effective than traditional Medicare. The idea behind lower payments seemed sound. Managed care had more flexibility with paying providers (i.e. using gatekeepers, demanding prior authorizations for tests, etc.), and managed care patients were in general healthier. Under these rules however, the private market was a relatively small slice of the total Medicare pie covering only 13% of all Medicare enrollees. The year everything changed was 2003. The Medicare Prescription Drug, Improvement, and Modernization Act (MMA) is best known for introducing prescription drug coverage to Medicare patients (Medicare Part D). Less well known is the provisions within the bill to provide a major increase in government contributions to private (Medicare Advantage) plans. As a result Medicare now pays more for private plans per enrollee (~$1,000) than the cost of care for beneficiaries in traditional Medicare. In 2014 payments to MA plans totaled ~$159 billion.
Regulatory Roundup
As of October 1, 2023, all 510(k) submissions, unless exempted, must be submitted electronically using eSTAR through the CDRH Portal, enhancing the quality of the premarket submissions and efficiency of premarket review
Thank you again for reading my newsletter.
If you enjoy reading this newsletter, please share it with someone else who might enjoy reading it.
Talk soon,
Hamid